Imagine this: you are out to dinner with a group of friends, and someone orders your favorite appetizer—bruschetta. As you take your first bite of this extra crispy bread sensation, you experience a sharp, intense pain in tooth #8, which is accompanied by the sound of a “crack.” At first you think that some idiot accidentally put a rock in the bruschetta. The truth of the situation, however, is that this was no rock; it was your crown that fractured to the gingival margin, leaving you toothless in front of your friends. Two thoughts cross your mind: “Great! How am I supposed to eat the rest of this bruschetta?” and “I know that I need to get an implant (because my general dentist always warned me about the fragility of this tooth and told me that an implant was the best solution), but I’ll have to wear some stupid flipper for 8 months!”
This scenario is not uncommon. It is funny, as I have surveyed many patients that have fractured a tooth, and the most common cause of such fractures is bread. I still believe that an implant is the best solution for most patients; however, over the course of my career, I have changed my treatment plan to include immediate provisional restoration (placement of an acrylic crown on the implant within a couple days of surgery) under ideal circumstances. I used to be scared of the potential risks of noncompliance and failure, but my experience and the literature do not support that fear. Don’t get me wrong—I still don’t trust the male species all that much when planning the treatment for these cases. I was once told by a prosthodontist that men are unreliable because most of them feel that if there is no pain from the implant surgery and a tooth is present, the immediate implant and provisional restoration can be used like a fully integrated implant or a natural tooth. Then again, I have had women who didn’t want to have immediate provisional restorations performed on their implants because they didn’t trust themselves either. I guess that I am damned with either sex.
According to two articles by Tarnow and Chu, there are eight benefits of immediate provisional restoration:
Advantages of Immediate Provisional Restoration
- There are fewer patient appointments overall.
- There is only one surgical procedure for the patient.
- The treatment time is shortened, as there is no need to uncover the implant (two staged procedure).
- A fixed provisional restoration is possible, as opposed to a removable appliance.
- There is an increase in patient comfort.
- The soft tissue can be sculpted with a tooth form rather than a cylindrical abutment.
- There is increased peri-implant soft tissue thickness.
- The alveolar bone can be preserved.
Tarnow and Chu et al.
When you think about it, the entire process is seamless. The patient’s maxillary and mandibular dentitions are digitally scanned before the tooth is removed. The tooth is atraumatically removed, and the implant is inserted to the appropriate torque value. The donor bone is placed in the gaps, and, if needed, a connective tissue graft is harvested and placed. A scan body is placed on the implant, and the area is digitally scanned. A stock healing abutment is then placed, and the digital file is sent to the dental laboratory for provisional crown fabrication. Either an Essex is given to the patient in the meantime, or, in most cases, the patient does not desire a replacement tooth at that time. The patient returns to the office 2-3 days later; the patient receives a numbing agent, and the provisional crown is inserted. The patient’s bite is checked, and the crown is modified to ensure that there is no occlusal contact. The patient is reminded multiple times and once more (especially if they are male) not to use this tooth under any circumstances; after that, the patient walks out happy. The patient is happy because everything was seamless and they don’t have to wear that “stupid” flipper. Over the next four months, not only is the bone consolidating around the implant, but the gingiva is healing around the provisional crown, allowing for the best outcome. More important, we have reduced the overall treatment time from nine to twelve months to four to five months, we have given a superior cosmetic result, and we have reduced the self-consciousness that some patients might feel while wearing a removable restoration. The only disadvantage is that we will still have to discourage the patient from eating bruschetta.
CASE: 57 year-old female presents to the office with pain on chewing for the last couple of months. She specifically points to tooth #12 as the culprit. The dental history for tooth #12 includes root canal therapy, post/core and crown. Clinically the tooth had a 6 mm periodontal pocket on the mesial and CT scan demonstrated bone loss on the mesial. Because tooth #12 had greater than 3mm beyond the apex to the sinus floor, the patient was an ideal candidate for extraction, implant, bone graft with immediate provisional restoration.
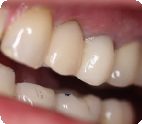
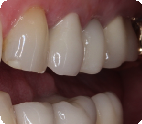

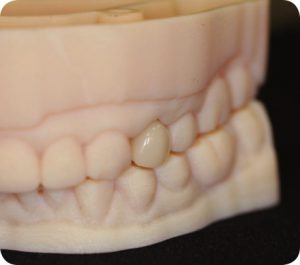
Matthew E. Dudziak, DDS, MD, MBA
Tarnow DP et al. Flapless Postextraction Socket Implant Placement in the Esthetic Zone: Part 1. The Effect of Bone Grafting and/or Provisional Restoration on Facial-Palatal Ridge Dimensional Change – A Retrospective Cohort Study. Int J Perio Rest Dent. Vol 34, #3, 2014. p 322-331
Chu SJ et al. Flapless Postextraction Socket Implant Placement in the Esthetic Zone: Part 2. The Effects of Bone Grafting and/or Provisional Restoration on Peri-implant Soft Tissue Height and Thickness – A Retrospective Cohort Study. Int J Perio Rest Dent. Vol 35, #6, 2015. p 803-809










